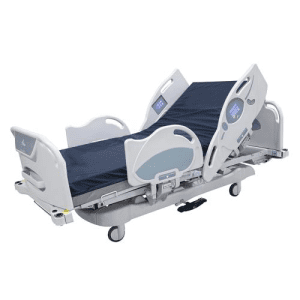
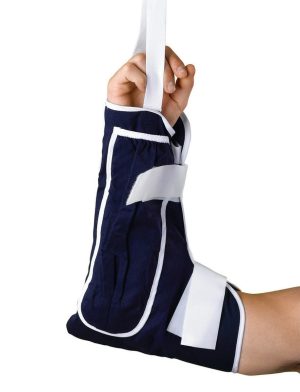
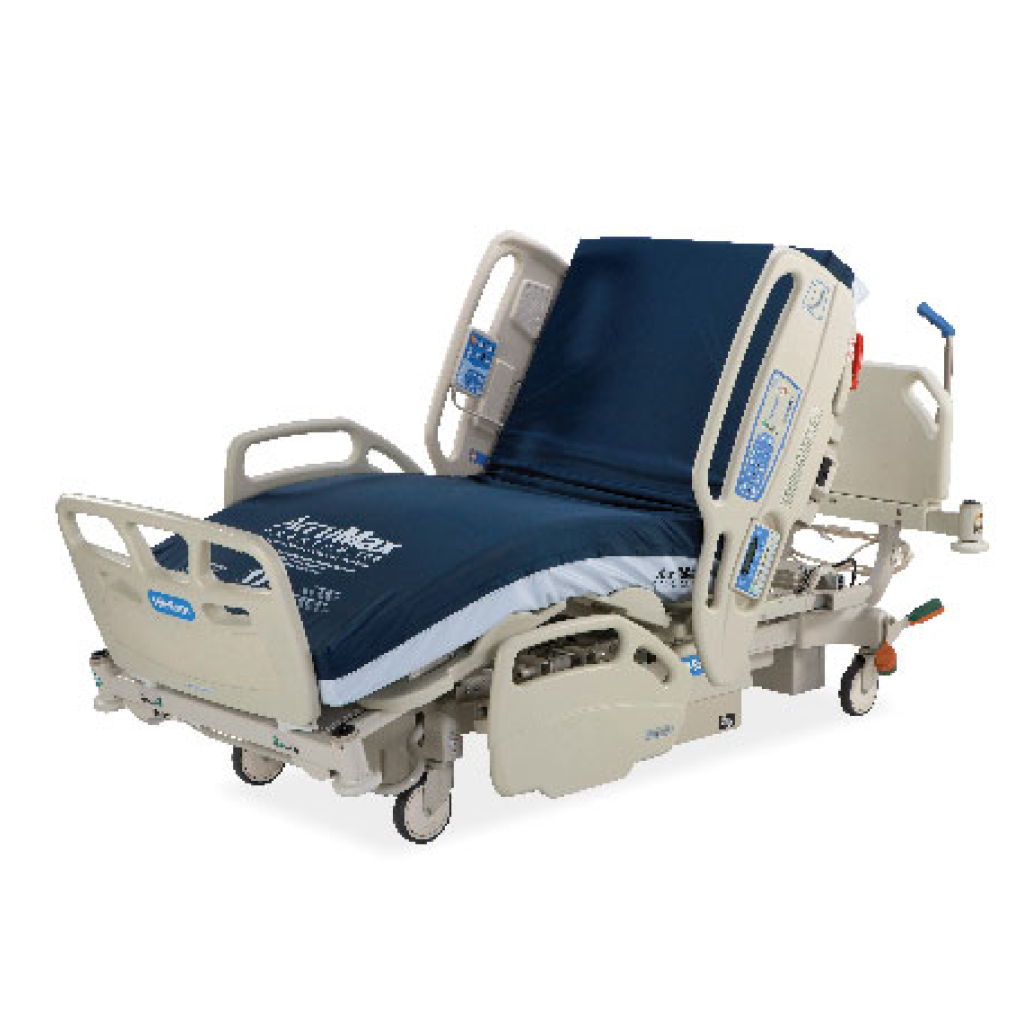
Product Highlights
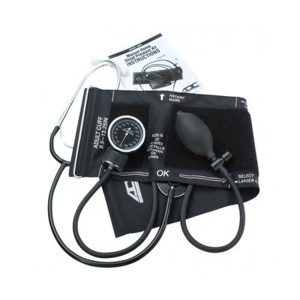
- 6016N Digital Wrist BP Monitor from ADC quickly measures systolic, diastolic pressure, and pulse with an auto off function to preserve battery life
- Smart Logic Technology determines ideal inflation levels and averages last 3 readings
- Internal memory recalls last 99 readings with date/time stamps for two users
- 6016N monitor includes a 5 Year manufacturer warranty








 Sign In
Sign In Contact Us
Contact Us